
More than 68 million infected with the novel coronavirus and more than 1.5 million dead. 2020 has been a year defined by global sickness and loss.
In the face of this extraordinary threat, it’s easy to forget how much we have accomplished. Doctors, nurses and staff in hospitals around the world have learned how to better care for those sick with COVID-19. Researchers have uncovered secrets of a virus that, not so long ago, was wholly unknown.
Accelerated efforts to create vaccines succeeded beyond even the most optimistic predictions, with the United Kingdom granting emergency use of a vaccine on December 2 and the United States poised to follow suit before the end of the year.
Meanwhile, public health officials have fought to inform the public about how to reduce the risk of infection amid an onslaught of false reports about cures and treatments, and denials about the pandemic’s severity. Millions of people have donned masks and dramatically reshaped their daily lives to help fight the virus.
In early January, we had no tests for detecting the virus, no treatments, no vaccines. And though we’re not where we want to be, we’ve made progress on all those fronts. But we still have so much to learn. Here are pressing questions that scientists seek to answer. — Emily DeMarco

Why do some people get sick while others don’t?
A person’s age and preexisting medical conditions are risk factors for more severe disease, and men appear to be at higher risk than women (SN: 4/23/20). But scientists don’t have many answers to explain the wide variety of experiences people have with SARS-CoV-2, the coronavirus that causes COVID-19. Many people have no symptoms. Some struggle to breathe, suffer strokes, or progress to organ failure and death.
People who develop severe disease do have something in common: “a very severe inflammatory response,” says cancer immunologist Miriam Merad of the Ichan School of Medicine at Mount Sinai in New York City. The body’s own immune response can get out of whack and inflict inflammatory damage in a misguided attempt to make things right (SN: 8/29/20, p. 8).
Scientists have begun to pick out immune system players that seem to gum up the works during a severe bout of COVID-19. For example, a problem can arise with type 1 interferons, proteins that kick off the initial immune response to an intruder and activate production of pathogen-destroying antibodies. Patients with severe COVID-19 can have a weak interferon response; in some patients, genetic errors can interfere with the production of interferons, in others, the immune system incapacitates the proteins (SN: 9/25/20).
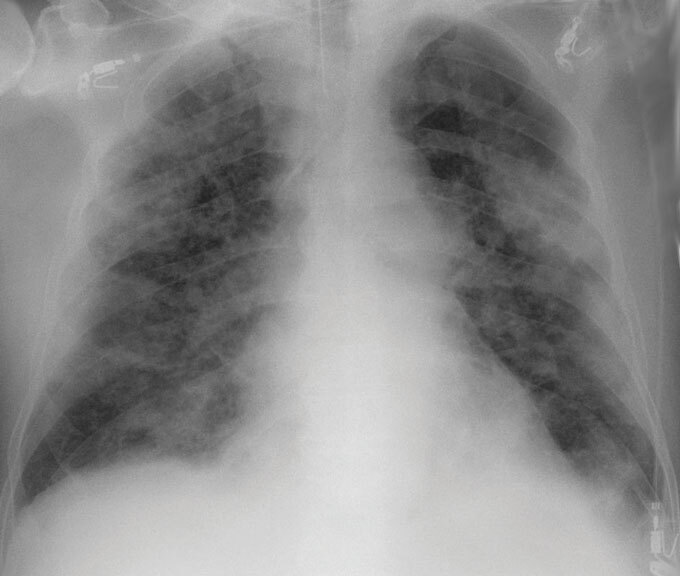
Meanwhile, some severely sick people produce an excess of other components of the body’s early immune response. In nearly 1,500 people hospitalized with COVID-19, Merad and colleagues measured four immune proteins that contribute to inflammation. High levels of two of the proteins, interleukin-6 and TNF alpha, predicted that a patient would go on to have severe illness and possibly die, even after accounting for age, sex and underlying medical conditions, the researchers reported in August in Nature Medicine.
It may be that people with no or mild symptoms have some degree of preexisting immunity. Some people who haven’t been exposed to SARS-CoV-2 have white blood cells called T cells that nonetheless recognize the virus. This appears to be due to past colds from common coronaviruses, researchers reported in October in Science. They speculated that this preexisting T cell immunity may contribute to differences in COVID-19 disease severity. — Aimee Cunningham
What are the long-term health consequences of an infection?
This question could take years to resolve.
For now, we know that for some people, the symptoms and suffering from COVID-19 can go on for months after the initial infection (SN: 7/2/20). There isn’t an agreed-upon definition for what some call “post-COVID syndrome” or “long COVID,” but symptoms tend to include fatigue, shortness of breath, brain fog and heart abnormalities. And these problems aren’t necessarily tied to a more severe initial illness.
It’s not yet clear how widespread the syndrome is or what to do about it. But studies are beginning to offer clues as to how common persistent illness is. Of 143 patients in Italy who had been hospitalized with COVID-19, 32 percent had one or two symptoms and 55 percent had three or more symptoms an average of two months after first feeling sick, researchers reported in August in JAMA. And in a survey of 274 symptomatic adults who had a positive test for SARS-CoV-2 but weren’t hospitalized, 35 percent were not back to their normal state of health two to three weeks after testing, according to a July study in Morbidity and Mortality Weekly Report.
One of the largest surveys so far comes from the COVID Symptom Study, in which people logged their symptoms into an app. Of 4,182 users with COVID-19, 13.3 percent had symptoms lasting more than four weeks, 4.5 percent had symptoms for more than eight weeks and 2.3 percent topped 12 weeks. The risk of persistent symptoms rose with age, researchers reported in October in a preliminary study posted at medRxiv.org.
To learn about the long-term physical and mental health effects of COVID-19, the U.S. National Institutes of Health plans to follow for months to years people who have been infected. And a trial by Steven Deeks, an internal medicine physician at the University of California, San Francisco School of Medicine, and colleagues will assess the role of inflammation in persistent health effects.
Long-term studies of entire communities will be especially important to learn how common persistent symptoms are, how long they last and why they’re happening, Deeks says. “Right now, we have just a whole long list of questions,” he says. “It’s going to take a lot to figure this out.” — Aimee Cunningham
How long might immunity last?
There are signs that the immune system can learn how to deal with the virus, bestowing at least temporary immunity. Most people appear to make immune proteins that stop SARS-CoV-2 in its tracks, called neutralizing antibodies, and also T cells that help coordinate the immune response or kill infected cells, says epidemiologist Aubree Gordon of the University of Michigan in Ann Arbor. Those antibodies and T cells can stick around in the body for at least six months, if not longer, studies suggest. “So that’s promising,” Gordon says.
But scientists don’t know how long a person will be protected from a future bout with the virus. “There’s just been a limited time for people to study this,” she says.
Still, SARS-CoV-2 is not the only coronavirus that infects people. For instance, four others that cause the common cold circulate around the globe. “We can get some evidence from what goes on with some of the human endemic coronaviruses,” says immunologist Brianne Barker of Drew University in Madison, N.J. For those viruses, protection lasts about a year. People can get infected with the same virus over and over again once their immunity wears off, though the severity of a second infection varies. The duration of immunity after an infection with the coronaviruses that cause SARS and MERS is unknown.
To date, there have been a few documented reinfections with SARS-CoV-2, suggesting that, for some, immunity doesn’t last very long. Efforts — including a study Gordon is working on — are under way to figure out how common reinfection really is and whether subsequent infections are any different from the initial one. — Erin Garcia de Jesus
What can we expect from the treatments and vaccines being developed?
Because of crucial advances in 2020, “we know more about the virus and some of the complications it causes and how to prevent and predict and treat those complications,” says Amesh Adalja, an infectious disease physician at Johns Hopkins Center for Health Security.
Doctors have learned tricks that help people breathe easier, such as putting hospitalized COVID-19 patients on their stomachs. And two drugs — the antiviral remdesivir and the steroid dexamethasone — have shown promise against the virus (SN: 6/16/20). The U.S. Food and Drug Administration approved remdesivir for use in hospitalized COVID-19 patients ages 12 and older in October because some studies showed that it can shorten hospital stays. But the drug, which is the only FDA-approved drug for COVID-19, didn’t reduce the chance of dying or going on a ventilator in a large study by the World Health Organization (SN: 10/16/20).
In November, the FDA gave a cancer drug called baricitinib emergency use authorization. In combination with remdesivir, the drug shaved an extra day off hospital stays compared with remdesivir alone in a large clinical trial. But many doctors aren’t convinced of baricitinib’s effectiveness.
Ideally, doctors could treat people before they are sick enough to need the hospital. Some drugs are in early stage clinical trials to determine if they can help people early in an infection (SN: 9/26/20, p. 8). Some antibodies taken from COVID-19 survivors and lab-made antibodies are also being put to the test (SN: 9/22/20). Lab-made antibodies from Eli Lilly and Company and Regeneron were given emergency use authorization in November for treating people newly diagnosed with COVID-19, making the therapies the first available to people who aren’t ill enough to go to the hospital. (Regeneron Pharmaceuticals is a major donor to the Society for Science & the Public, which publishes Science News.)
Vaccines are being developed on a fast track. Russia was the first country to announce it had a vaccine for the public, though scientists question its efficacy (SN: 8/11/20). China has also given the nod for emergency use of some vaccines for the military (SN: 8/1/20, p. 6) and general public, although those vaccines are still in testing too. The United Arab Emirates authorized two vaccines made in China for use by its citizens.
Both Pfizer and Moderna announced in November that their mRNA-based vaccines were about 95 percent effective at preventing illness (SN: 11/16/20; SN: 11/18/20). On December 2, the United Kingdom OK’d Pfizer’s vaccine for emergency use, making the vaccine the first to get the nod after thorough testing. AstraZeneca and the University of Oxford reported that their vaccine prevents illness too, and may cut down on transmission of the virus (SN: 11/23/20).

Over 200 other vaccines are in development worldwide, says Esther Krofah, executive director of FasterCures, part of the Milken Institute think tank. But getting doses of a vaccine, at least initially, “will not be as straightforward as calling up your local CVS,” she says.
In the United States, 21 million health care workers and about 3 million people living in long-term care facilities are expected to be first in line for the vaccines (SN: 12/1/20). Children may be among the last to be immunized. That’s because vaccines haven’t been tested in kids under 12, and children are less likely to die or develop severe disease than adults.
Bottom line: A COVID-19 vaccine may not be widely available in the United States until late spring or summer 2021.
Even when a vaccine is approved for broad use and there’s a large enough supply, “the bigger challenge will come in distributing vaccines widely,” says Julie Swann, a health systems engineer at North Carolina State University in Raleigh. Pfizer’s vaccine, for instance, has to be kept frozen at supercold temperatures. So distributors must either be able to give out all of their doses within a couple of days after receiving a shipment, or have access to special freezers or dry ice to keep the vaccines cold enough. Big cities may have more access to those measures than rural areas.
Many of the vaccines in testing require two doses. Keeping track of who has gotten which vaccine and when it’s time for a booster, and whether booster shots are available, could also be challenging, Swann says. — Tina Hesman Saey
Will the pandemic end in 2021?
“I don’t think anyone can say with clarity what the end of the pandemic might look like,” says Michael Osterholm, an epidemiologist at the University of Minnesota in Minneapolis. If a vaccine can confer long-lasting immunity, on the order of years to decades, widespread community transmission around the globe could cease, he says.
But “a vaccine is nothing until it becomes a vaccination in somebody’s arm,” Osterholm says. And those arms must be willing. Vaccine development has progressed at a record pace, but some experts worry that speed, and the politicization of certain drugs, have seeded distrust (SN: 8/1/20, p. 6). “Acceptance is going to be a huge issue,” he says.
Of course, many countries managed to slow the virus’ spread without a vaccine. In the United States, “we don’t have to wait to get this under control,” says public health researcher Megan Ranney of Brown University in Providence, R.I. “We already know that basic, multimodal public health interventions work.”
Such interventions include widespread and easily accessible testing that spurs contact tracing and case isolation, as well as consistent public health messaging around the importance of wearing masks, social distancing and avoiding crowded indoor spaces.

Thus far in the United States, these basic public health interventions have been patchy and inadequate on a national scale (SN: 7/1/20). That’s allowed the “first wave” of infections to slosh around the country, growing in size to about 200,000 new cases each day in early December. Whether this dire trend worsens in the early months of 2021 depends in large part on federal action, both Osterholm and Ranney say.
“We need a national plan, and we don’t have a national plan,” Osterholm says. That may change with the election of Joe Biden, who campaigned on creating a coronavirus national plan. Osterholm is part of the president-elect’s Transition COVID-19 Advisory Board, which has begun planning a new federal response.
Broadly, that plan includes clear and consistent public health messaging, a well-funded national testing strategy, support for states to boost contact tracing, supplying personal protective equipment to essential workers and mask mandates. “If we have all those things in place, the coming year could be somewhat similar to where we’ll be with widespread vaccination,” Ranney says. People could go about most normal activities with a little extra caution, wearing masks and avoiding crowds indoors.
Still, measures like universal mask wearing, social distancing and contact tracing only work if people abide by them. As the pandemic wears on, experts worry that complacency and fatigue could further fracture an already uneven response to the disease.
If the United States “continues on the path we’re on now, we’re going to continue to see increasing numbers of people hospitalized and dead, continue to go through this seesaw of full lockdown then full reopening, confusing messages, unmitigated anxiety and fear and a worsening economy,” Ranney says. — Jonathan Lambert
Once the pandemic ends, will the virus still circulate?
When the pandemic eventually fizzles out, the coronavirus itself will probably stick around for a while, experts say. How long, however, depends on how well our immune system and available vaccines protect us from reinfection.
So far, it’s impossible to say how frequently reinfections with SARS-CoV-2 happen based on the small number of these cases identified. But if reinfections become common in the face of waning immunity, then the virus is likely here to stay.
For example, if immunity lasts around 40 weeks, as it does for some cold-causing coronaviruses, then there may be yearly outbreaks of COVID-19, researchers reported in May in Science. If the immune system’s memory of the virus lasts slightly longer, say two years, then there may be biannual outbreaks. Permanent immunity could mean the virus may disappear entirely, though that possibility is unlikely since respiratory viruses like influenza and viruses that cause colds rarely lead to this sort of long-lasting immunity.
Adding an effective vaccine to the mix would help build — and maintain — immunity among people to control potential future outbreaks. And if a vaccine is highly effective and enough people take it plus any boosters or follow-up vaccinations as needed, that could help prevent the virus from spreading at all. But those are big ifs.
Because SARS-CoV-2 can be spread by people without symptoms, some experts do not anticipate the virus will go away any time soon, unlike the coronavirus that caused SARS. That virus stopped circulating among people a little more than a year after it appeared, in part because it wasn’t spread by people with no symptoms. That allowed public health experts to more easily isolate sick patients and quarantine their contacts to prevent the virus’ spread. It’s estimated that around 30 percent of people infected with SARS-CoV-2 don’t show symptoms, making such total containment much harder.
“From everything we’re seeing so far,” says Barker, the Drew University immunologist, “this virus may become endemic and may be with us for a long time.” — Erin Garcia de Jesus

 A new treatment could restore some mobility in people paralyzed by strokes
A new treatment could restore some mobility in people paralyzed by strokes  What has Perseverance found in two years on Mars?
What has Perseverance found in two years on Mars?  This robot automatically tucks its limbs to squeeze through spaces
This robot automatically tucks its limbs to squeeze through spaces  Greta Thunberg’s new book urges the world to take climate action now
Greta Thunberg’s new book urges the world to take climate action now  Glassy eyes may help young crustaceans hide from predators in plain sight
Glassy eyes may help young crustaceans hide from predators in plain sight  A chemical imbalance doesn’t explain depression. So what does?
A chemical imbalance doesn’t explain depression. So what does?